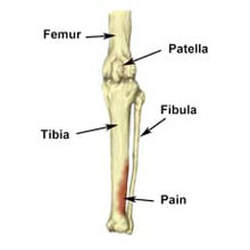
 Medial Tibial Stress Syndrome (MTSS) is a common musculoskeletal condition associated with running and walking activities. Recovery times in MTSS range greatly, but tend to be long – 4 weeks to 18 months in some cases. For this reason, it is something to spot and treat early. Let’s look at MTSS more closely: The tibia bone is the larger of the two bones in your lower leg; Medial refers to the inside part of the leg; and Stress refers to the forces, or loads, applied to the body. Quite simply, MTSS is thought to be a consequence of mechanical overload; when the capacity of the tissues (the tibia bone for example) is outweighed by the load and demands placed upon it: causing injury. The phrase ‘shin splints’ has been used for a long time to describe pain vaguely localised around the shin. Interestingly, ‘shin splints’ is a term that in fact doesn’t help our understanding of lower leg pain at all – not only has it been used to describe MTSS, it also refers to other similar clinical presentations of pain, such as: stress fractures of the tibia or fibula; chronic compartment syndrome; and ischemic shin pain, to name a few. ‘Shin splints’ can contribute to confusion in understanding the cause or causes of MTSS, which doesn’t help those researching it – so it may well be a phrase of the past quite soon. MTSS is often reported to include strain on the muscles and other tissues around them (myofascial strain), inflammation of the tibia bone itself (periostitis) and bone stress. Pain usually comes on suddenly linked with an increase in training load, is worse with exercise, and is alleviated with rest. The pain is usually localised to the medial bottom third of the tibia, spreading at least 5cm in distance. MTSS is debilitating and can be a frustrating condition to get over, with no ‘gold standard’ treatment identified as of yet, but there are certainly things we can do. Running is an enjoyable, liberating form of exercise that only requires some basic tips to help steer away from potential injuries like MTSS. Here’s one of my favourite tips for runners: Monitor 3 key training variables: distance; speed; and incline. Gradually increase one variable at a time and slowly build your body’s capacity to do more. Be mindful that doing too much, too quickly, can be a risk factor for MTSS and over conditions. The team here at Physioimpulse can help advise how to prevent, treat and manage Medial Tibial Stress Syndrome, with hands on techniques and rehab whilst also exploring your training plans and assessing for load:capacity mismatches. Good luck and stay active! Chris, PhysioImpulse Bath Physio 01225 683007References
Becker, J., James, S., Wayner, R., Osternig, L. and Chou, L.S., 2017. Biomechanical Factors Associated With Achilles Tendinopathy and Medial Tibial Stress Syndrome in Runners. The American journal of sports medicine, 45(11), pp.2614-2621. Newman, P., 2016. Medial Tibial Stress Syndrome (Doctoral dissertation, University of Canberra). Winters, M., Backx, F.J.G., Franklyn, M., Moen, M.H., Weir, A. and Bakker, E.W.P., 2016. The medial tibial stress syndrome score: item generation for a new patient reported outcome measure. South African Journal of Sports Medicine, 28(1), pp.11-16.
1 Comment
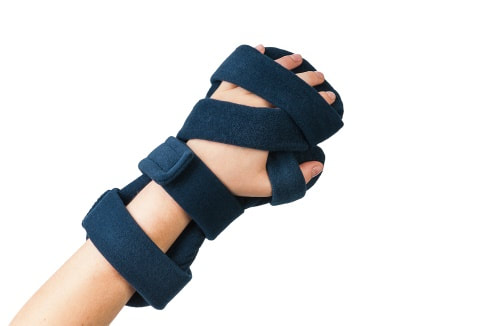
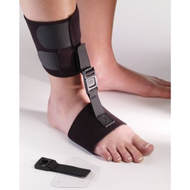 Orthotics are appliances that are used to improve the function, alignment and mobility of a particular area of the body. These include splints, ankle-foot-orthoses (AFOs), braces or insoles. The NICE guidelines recommend that patients with a neurological condition should be considered for an orthotic assessment as early as possible to promote optimal independence and function. They can also reduce pain and improve a person’s confidence. Here are a few commonly used orthotics: Lower Limb Ankle- foot-orthosis
Please get in touch if you would like an assessment from our specialist neurological physiotherapist to advise on the best orthosis for you.
Thinking of starting running but don't know where or how to start? The NHS Choices 'Couch to 5k' is a free running plan for absolute beginners helping you gradually work towards running 5km in just 9 weeks!
Running has so many health benefits such as:
https://www.nhs.uk/LiveWell/c25k/Pages/couch-to-5k.aspx Bath Physio Specialists 01225 683007A stroke is a sudden neurological event caused by a clot in the blood vessels supplying the brain (ischaemic stroke) or a bleed in the brain due to weakened blood vessels (haemorrhagic stroke). Both types of stroke restrict blood supply and oxygen to brain tissues and can cause a variety of different symptoms. These include:
Neurological Physiotherapy at Physioimpulse Our specialist and experienced neurological physiotherapists can help to maximise your recovery and potential following a stroke. Our physiotherapists are able to use a number of specialist treatments to ensure you can reach your rehabilitation goals and regain independence as soon as possible. Physiotherapy treatment may include:
Martin was a very active man in his mid 40’s who loved any outdoor adventure sports including rock climbing, mountaineering and bouldering. He was highly successful in his career and owned a small advertising company, which he thoroughly enjoyed. Martin had a left middle cerebral artery stroke (MCA), which meant that the right side of his body was affected. Initially his main symptoms were:
Early days Martin spent a total of 10 months in hospital, which included time in an acute stroke unit and then in a neuro-rehabilitation unit. During this time, some progress was made and Martin started to use an electric standing hoist to be transferred from his bed to the chair. This meant that his right leg had sufficient power in it to be able to take weight through it when using the hoist with the carers. His right arm had started to be able to joint in with daily tasks such as eating and washing but needed assistance. Unfortunately, as Martin’s progress was relatively slow, he was discharged to a nursing home after 10 months of rehabilitation and looked after by carers 24 hours a day. Martin had been severely affected by fatigue but after 6 months in the nursing home, decided to start physiotherapy again to see if any further progress could be made. Our specialist neurological physiotherapist, Katie, started seeing Martin twice a week at the nursing home. A thorough assessment was carried out and a treatment plan and individualised goals were set between them. Treatment varied and included:
After another 6 months, Martin was able to stand independently and step around to a chair using a specialist quad stick for support. He had also started taking a few steps. 1 year on Martin’s mobility and balance progressed to such an extent that he was able to return home after a year of being discharged to the nursing home. He initially needed carers 3 times a day to support with showering, meals and shopping and was independent with all of his transfers and mobility including his stairs. He is now independent with all of his activities of daily living and just has a cleaner to help with his housework once a week (which he is very pleased about!). Martin can drive an adapted car and go out independently to meet friends and socialise. He is still continuing with physiotherapy, which now even include sessions in the local climbing centre! It is often reported that recovery gains start to significantly slow down after 6 months following a stroke and no further changes can be made after 2 years. Martin’s story is an important example that everyone should be treated as an individual rather than a statistic. In the right environment and with specialist rehabilitation, improvements can continue to be made for many years. Bath Physio 01225 683007 |
AuthorPhysioimpulse Chartered Physiotherapists Archives
June 2024
|
Services |
Get in Touch
|
©



 RSS Feed
RSS Feed

