Costco-vertebral joint irritation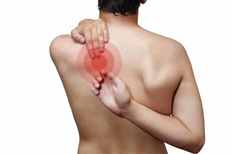 Costco-vertebral joint irritation is pain originating from where your ribs attach on to the spine in the centre of your back. It’s a common place to suffer with pain, in particular for desk workers who are hunched forward for the majority of the day. It will be the area which you can never reach, between the shoulder and the neck but slightly too far down to show someone the exact point which is causing the pain. Bath Chiropractic 01225 683007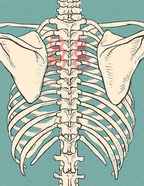 The most common presentation with someone suffering from this injury is pain between the shoulder blades, which doesn’t seem to improve with massage or stretching. If left for longer than a few weeks, the pain can start to travel into the neck and head, in addition to shoulder pain and restriction. This joint where the rib attaches to the spine needs to move when we breathe, so when the costo-vertebral joint can’t move freely it can be painful during deep breaths or lying on the painful area at night. In unusual circumstances this can present as chest pain, where the ribs can’t move properly and the pain wraps around to the front of the chest. By assessing and detecting the painful region, Chiropractic treatment including spinal manipulation can relieve the symptoms and increase the movement to the affected joint and the surrounding area, relieving the pin-point tenderness and any associated head, neck or shoulder symptoms. By addressing the primary cause, the muscles sitting on top or surrounding the irritable joint will overtime desensitise and stop tensing to protect the injured area. Like with most injuries, icing the area will reduce excess inflammation to a muscle, and specific exercises can help prevent future recurrences. If this sounds like something you suffer with, don’t hesitate to contact us and book in with our Chiropractic team
0 Comments
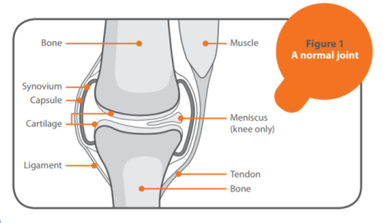
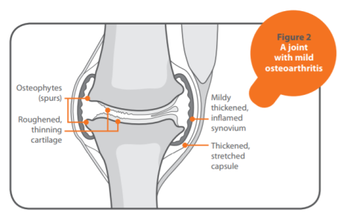
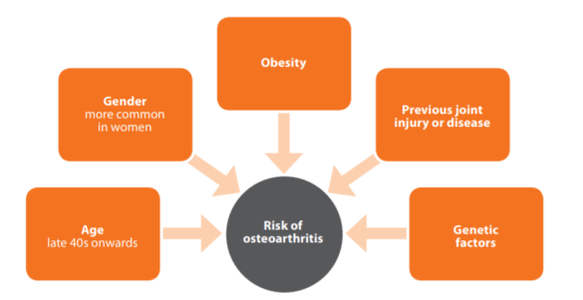
Osteoarthritis: Exercise as Medicine For people with hip and knee osteoarthritis (OA), high-quality research shows that exercise therapy is very helpful in decreasing pain and improving movement in these joints. The phrase, Exercise as Medicine, has been used for some time – but not just for OA, for some twenty five other long term health conditions too. OA is the most common cause of arthritis and a major public health problem. It was first thought of as simply ‘wear and tear’ affecting cartilage within joints. Common misbeliefs focused solely on mechanical (load-related) or occupation-related reasons for these joint changes. However, our knowledge of this condition has advanced considerably. OA is a condition mediated by and affecting the entire ‘synovial joint organ’, which means it affects much more than just cartilage. It includes not only fibrocartilage and hyaline cartilage, but also the bone below this area (subchondral bone) and the soft tissue which lines the joint (synovium). More recently, a central theory of the cause of OA is that of chronic, low-grade inflammatory processes not only promoting OA symptoms, but also accelerating OA progression. Many risk factors come into play when considering the cause of OA, as outlined in the Arthritis Research UK information leaflet. 01225 683007(ARUK 2018) Exercise as Medicine It is widely known that exercise should be an integral part of standard care for people with knee and hip OA. Raising your physical activity levels is effective in achieving good outcomes. Exercise should consist of:
There are also many other important non-surgical treatment options available to those who suffer with OA. At Physioimpulse we have a Gait analysis and Biomechanic assessment service which enables us to assess your foot mechanics and create custom made insoles to reduce the pain of OA affected joints and enable more effective rehabilitation. Some people struggle to exercise efficiently due to high pain levels so we also provide Ostenil injections which"lubricate" the joint and can provide up to 9 months of pain relief. Other Non-Surgical Treatment Options
Here at PhysioImpulse, we want to support you to keep active and manage your OA as best able. Take home Message: Stay active and exercise! Bath Physiotherapy 01225 683007Tumeric Pills
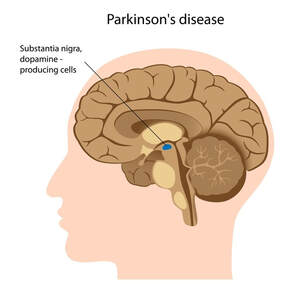
https://webmd.com-us.health/diet/health-benefits-turmeric References Arthritis Research UK (2018) https://www.arthritisresearchuk.org/arthritis-information/conditions/osteoarthritis.aspx [Accessed online 2nd September 2018] Exercise Is Essential for Osteoarthritis: The Many Benefits of Physical Activity Journal of Orthopaedic & Sports Physical Therapy, 2018 Volume:48 Issue:6 Pages:448–448. Liu-Bryan, R. and Terkeltaub, R., 2015. Emerging regulators of the inflammatory process in osteoarthritis. Nature Reviews Rheumatology, 11(1), p.35. Osthoff, A.K.R., Niedermann, K., Braun, J., Adams, J., Brodin, N., Dagfinrud, H., Duruoz, T., Esbensen, B.A., Günther, K.P., Hurkmans, E. and Juhl, C.B., 2018. 2018 EULAR recommendations for physical activity in people with inflammatory arthritis and osteoarthritis. Annals of the rheumatic diseases, 77(9), pp.1251-1260. Pedersen, B.K. and Saltin, B., 2015. Exercise as medicine–evidence for prescribing exercise as therapy in 26 different chronic diseases. Scandinavian journal of medicine & science in sports, 25, pp.1-72. NICE guidelines support physiotherapy for patients with Parkinson’s Recently updated NICE (National Institute for Clinical Excellence) guidelines have suggested that individuals with a diagnosis of Parkinson’s should have an assessment from a specialist neurological physiotherapist and on-going access to physiotherapy. NICE advocates that physiotherapy can help to manage symptoms and maintain an independent lifestyle. It can also reduce the number of admissions into hospital. NICE quality statement (updated February 2018) Adults with Parkinson's disease are referred to physiotherapy, occupational therapy or speech and language therapy if they have problems with balance, motor function, activities of daily living, communication, swallowing or saliva. NICE also advises early input after a diagnosis of Parkinson’s from a specialist physiotherapist in this field. This can help people to keep in control of their condition and symptoms and allow them to live well and independently with Parkinson’s. This recommendation was updated in 2017 and highlights the benefit that physiotherapy can contribute to in the management of Parkinson’s short and long-term. Parkinson’s is a progressive neurological condition, which affects an area of the brain known as the substantia nigra. This area normally produces a chemical known as dopamine, which helps to control the coordination of movement. In Parkinson’s, the nerve cells in the substantia nigra become damaged meaning that dopamine production is reduced. This can cause symptoms such as tremors (shaky movements), slowness of walking and rigidity (stiffness in muscles and joints). Other common symptoms are freezing (feet feel ‘stuck’ to the ground), falls, speech and swallowing difficulties and pain. Bath Neuro Physio |
AuthorPhysioimpulse Chartered Physiotherapists Archives
June 2024
|
Services |
Get in Touch
|
©

 RSS Feed
RSS Feed

